As a charitable organization connected to over 2,800 young mental health advocates across the country, we are in a prime position to provide information on the youth mental health experience in Canada. Jack.org has always engaged young people, worked with them to tackle complex mental health issues in their community, and listened. Now, we're sharing what we've heard.

Download the full 2019 Youth Voice Report
Meet the Network
Our network is made up of over 2,800 young leaders: nearly two-thirds (61.4%) of the youth in our network report having had a mental health struggle. Almost a quarter of our network (21.5%) identify as members of a visible minority group and slightly fewer (17.8%) as members of the LGBTQ2S+ community. The majority (70%) live in cities, both large and small, some (26%) live in suburban areas, and fewer (4%) live in rural areas.
But they are much more than the numbers. They are rigorously trained in mental health advocacy and are leaders within their communities. They've been working tirelessly to tackle barriers to positive mental health for their peers by improving knowledge and changing attitudes. This year alone, they will deliver more than 550 Jack Talks in every province and territory in Canada. 285 Jack Chapters will stage over 1,000 initiatives that will directly impact 130,000 of their peers. And they’ll host over 30 Regional Summits, bringing together 2,145 advocates within their communities to amplify their impact.
But there are limitations to the scope of peer-to-peer advocacy; increasingly, young people in our network have drawn attention to the fact that there are some mental health challenges they cannot tackle alone. For instance, while our network can raise awareness about mental health on campus and the services available, they can do little on their own to change the reality of wait times to access services. They need the support of adult decision-makers in order to change both systems and policies.
The State of Youth Mental Health in Canada
In 2015, a staggering 518 youth aged 15 to 24 years died by suicide in Canada. A further 150,000 attempted suicide, and as many as one in seven reported having suicidal thoughts. In Canada, one in five young people have at least one diagnosable psychiatric disorder, and more than 70% of psychiatric illnesses that carry significant morbidity risks in adulthood have their onset in childhood and adolescence. Yet, according to the Mental Health Commission of Canada, only 20% of these young people will receive appropriate treatment.
An Ontario study found that a quarter of children and youth waited three months for a consultation with a mental health specialist. These bottlenecks result in young people with mental health struggles not receiving support in a timely manner and, as their mental health struggles worsen, only receiving support in times of crisis. In Ontario, between 2012 and 2014, 40% of mental health care visits for young people and children were in an emergency setting.
The Process
Over the last year, we’ve gathered feedback from our network on how adult allies can better support youth mental health. To start, we surveyed 541 members of our network when they registered for our Jack Talks and Jack Chapter programs. We asked them two questions: 1) What creates mental health struggle among young people? And 2) What prevents young people from seeking help? We also ran focus groups at our Jack Summits and Regional Jack Summits, asking mental health advocates all over the country what they would ask of adult decision makers to advance youth mental health both in their communities and nationally. We also had help from ten Jack Chapters at post secondary institutions across Canada. These Chapters took part in the Campus Assessment Tool pilot, working with administrators and surveying a total of 1,124 of their peers to understand the strengths and challenges associated with their local mental health systems.
Some Key Findings
• The vast majority (81%) of young people we surveyed cited academic stress as a major cause of mental health struggle for both themselves and their peers.
• Over half (54%) of those we surveyed cited social media as a major cause of mental health struggle for both themselves and their peers.
• Close to three quarters (74%) of our network reported that their peers didn’t know when or where to get help, nearly as many (72%) said young people in their community didn’t know what types of mental health services were available, and over half (62%) cited difficulty in navigating the mental health system as a barrier that young people face when trying to get help during struggle.
• While the majority of young people surveyed don't hold stigmatized views of mental health, mental illness, or help seeking themselves, many of them still believe their peers hold these views. For example, when asked if they personally would think differently of a friend if they knew they sought mental health support, a very small minority (6.1%) of students agreed, but when asked if they feel fellow students would think differently of them if they knew they sought mental health support, far more (41.2%) agreed.
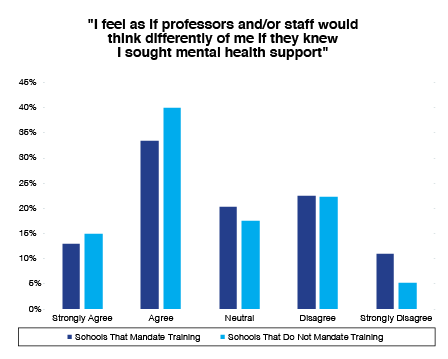
• Overall, almost half (48.9%) of all students surveyed agreed that faculty and/or staff would think differently of them if they knew they sought mental health support. However, when comparing institutions where faculty and/or staff receive mandated mental health training to institutions where such mandates don't exist, the value of basic mental health training becomes clear. On campuses where training was mandated, fewer students (46.9%) felt that faculty and/or staff would think differently of them if they sought mental health support. On campuses where training was not mandated, more students (54.9%) felt that professors and/or staff would think differently of them for seeking help when they needed it.
• In comparing schools that offer student health care plans, we found that coverage rates vary widely: a student at McGill University would receive 80% coverage up to $500 per year in psychological and counselling services, while a student at Dalhousie University would receive full coverage up to $1000 in the same period of time.
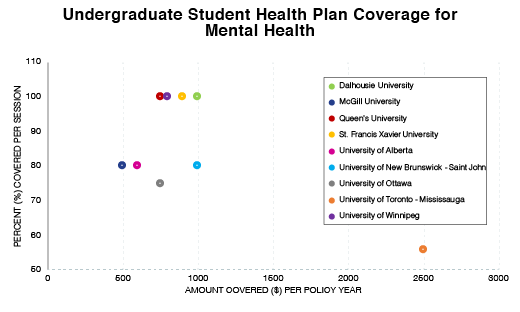
Percent (%) covered per session for the University of Toronto, Mississauga was calculated using the suggested hourly rate ($225/hour) for psychological services, determined by the Ontario Psychological Association.
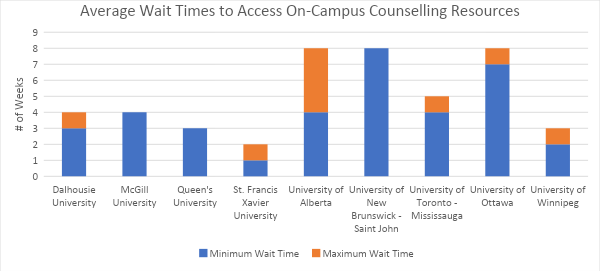
• All ten post-secondary campuses that took part in the Campus Assessment Tool pilot have a designated counselling centre that offers on-campus services to students who may not be going through crisis, but do require some form of support. Most students who want to access these services face wait times that range from 1 to 8 weeks, and the average wait time across all Campus Assessment Tool pilot campuses was 4 weeks.
Recommendations
After having undergone this research and consultation, a clear set of recommendations to guide adult decision-makers on how to promote youth mental health emerged. These five key recommendations are:
1. Protect, promote, and maintain positive youth mental health on campuses by offering a broad range of mental health resources including: crisis management services, ways to identify and respond to early signs of mental health struggle, and by applying a mental health lens to all policies, programs, and practices. This 360 degree approach that addresses mental health struggle from promotion to prevention will better meet the needs of a diverse youth population.
2. Consult students on what changes to the education system or at specific institutions would positively impact their mental health. As mentioned, 81% of those we surveyed cited academic stress as a cause of mental health struggle for both themselves and their peers. We must be open to reevaluating our education system, specifically the processes of how we instruct and assess students, to alleviate mental health struggle among young people while still maintaining our high standards of education.
3. Ensure social media better promotes mental health. For those who work with young people, this means researching and developing guidelines for young people on how to navigate social media in healthy ways. For those who work in social media, this means researching and creating a digital environment that fosters positive mental health, and sharing learnings with the community along the way. As mentioned, 54% of those we surveyed cited social media as a reason for mental health struggle for both themselves and their peers.
4. Deliver services that meet young people’s unique needs by engaging young people in discussions of how to deliver mental health services, collecting mass feedback and, especially in health care settings, involving young people in key decisions that impact their mental health. Mental health and health care services in general cannot expect to meet the needs of, and engage young people, without meaningfully consulting young people in the development process.
5. Support young people in navigating an extremely complex mental health care system, so they can find and access care that meets their needs in a timely fashion.
A Call to Collaboration
Young people are already incredibly motivated to change the state of mental health in Canada; here at Jack.org we consistently witness their resourcefulness and perseverance when faced with challenges to their mental health. Adult decision-makers are uniquely positioned to introduce policies that support them and promote mental wellbeing. It’s our sincere hope that these recommendations will be used to guide them to implement forward-thinking policies. Creating these changes is essential to the health of our country. Let's join forces, share ideas, and work together.
Download the full 2019 Youth Voice Report